By Kendall Watson, Physician Home Page Lead, Mid-Atlantic Permanente Medical Group
The Mid-Atlantic Permanente Medical Group Department of Imaging Services is pleased to announce that, in conjunction with the Departments of Endocrinology, we have begun offering Outpatient I-131 Therapy for Thyroid Cancer at the Tysons Corner Medical Center and Largo Medical Center, with plans to provide this service at the South Baltimore County Medical Center in the near future. A tremendous amount of thought has gone into internalizing this complex service, building upon the successes of our Regional I-131 Therapy Program for Graves Disease and other hyperthyroid disorders.
While not as prevalent as breast or colorectal cancer, thyroid cancer has an age-adjusted incidence rate of 11 per 100,000 persons, with over 56,000 cases projected to be diagnosed in the U.S. in 2017. It is considered a “common cancer,” by The National Cancer Institute. It is one of the fastest growing cancer diagnoses in the USA, with a 6.2% annual percentage change from 1997 to 2006. Of note, the disease incidence is 2.9-times higher in women. It has been hypothesized that reproductive, menstrual and environmental factors may account for this disparity, but very little is known about what specific factors account for this gender difference. The mortality rate of thyroid cancer, however, is lower than other cancers, especially if it is detected and treated at an early stage.
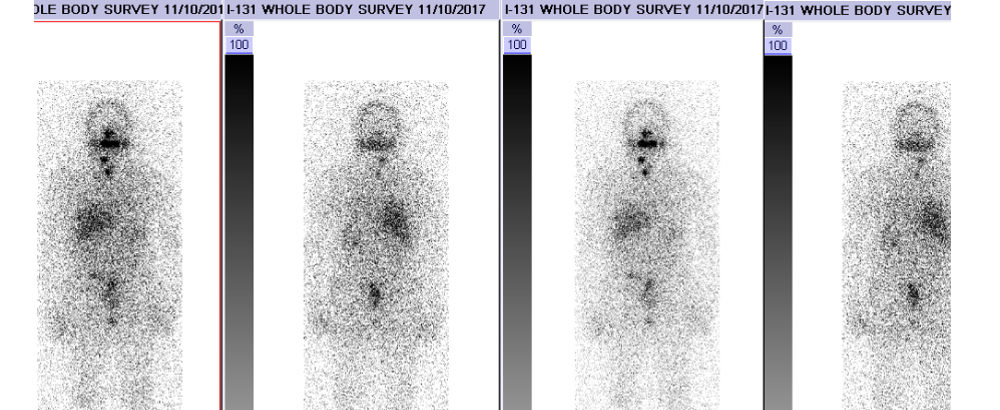
An established treatment for thyroid disorders since the 1940s, I-131 (radioactive iodine) therapy is a particularly effective way of treating the majority of thyroid cancers (differentiated thyroid cancer) when paired with surgery. Residual differentiated thyroid cancer cells are irradiated because they concentrate the radioactive isotope with minimal effects on the rest of the body.
Internalization of this procedure will help MAPMG reach its goal of decreasing external referrals for I-131 treatment by 80% or more in 2018. MAPMG physicians, working within the framework of Kaiser Permanente’s model of integrated medicine, are well-positioned to internalize this multidisciplinary procedure. After our expert surgeons have removed the cancerous thyroid tissue, Endocrinologists work with Radiology’s Nuclear Medicine sub-specialists for proper dosing of I-131, and ensure adherence with post therapy radiation safety precautions. “By internalizing this procedure, the patient’s care is not fragmented,” stated Nuclear Medicine Subspecialty Chief Vincent Dam, MD. So far, two patients have undergone treatment since the program was launched on Oct. 17.
MAPMG extends our gratitude for the expertise and partnership of our team of Nuclear Medicine sub-specialty chiefs: Dr. Vincent Dam, Howard DiPiazza, MD, and Phil Mulugeta, MD, together with Lida Tabatabaeian, MD from the NOVA Endocrine Department, in developing such an effective treatment protocol for our members. “This newly internalized procedure creates tremendous value for our patients, who can now have their I-131 treatments done as an outpatient, at their familiar Kaiser Permanente Medical Centers, by MAPMG physicians who they know and trust” stated Ainsley MacLean, MD, Regional Co-Chief of Imaging Services.
Pre-therapy consultations with our Nuclear Medicine Radiology Specialists are available at the Gaithersburg Medical Center, with subsequent I-131 treatments scheduled at Tyson’s Corner Medical Center or Largo Medical Center. Video visits for the consultation will be coming shortly.