In an effort to always continue improving patient care, MAPMG behavioral health professionals treating depression now have another tool for patients who aren’t responding to traditional treatments like prescription drugs.
Last September, we began offering a promising high-tech depression therapy at Northwest D.C. Medical Center Behavioral Health Clinic called Repetitive Transcranial Magnetic Stimulation, or rTMS.
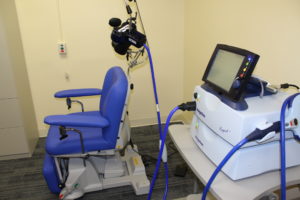
A non-invasive neuromodulation therapy, rTMS involves sending painless magnetic pulses through the brain. Specially-trained physicians and medical staff do this by placing a small device on the outside of the head. rTMS results in changes to chemicals in the brain, which may reduce symptoms of depression.
The program, under the leadership of Associate Medical Director B. Rao Tripuraneni, MD, is administered by MAPMG psychiatrist Frederick Wu, MD. Dr. Wu completed a visiting fellowship in TMS at Duke University, and performs the initial titration session. Specially-trained nurses and clinical assistants work together to perform the rTMS procedure and monitor for seizures, which are a very rare side-effect.
“The Mid-Atlantic region is expanding our ability to offer these tools to treat patients with treatment-resistant depression,” said Dr. Tripuraneni. “There’s a group of our patients who could truly benefit from this treatment option.”
TMS has been slowly growing in popularity since the FDA cleared the first TMS devices in 2008 for the treatment of major depression in adults who had failed to improve after at least one round of drug therapy. A growing body of evidence suggests that the effectiveness of rTMS may be comparable to antidepressant medications.
“Psychiatric treatments, on the whole, have response rates that aren’t that great,” said Dr. Wu. “The more options that we have, the better for our patients.”
Until recently, when patients suffering from major depression fail to respond to multiple courses of antidepressants, behavioral health professionals faced the choice of either prescribing ever-stronger medications or recommending Electroconvulsive Therapy – which is still considered the “gold standard” for severe depression, when indicated.
Magnetic stimulation is aimed at patients with such “treatment-resistant depression,” according to the federal Agency for Healthcare Research and Quality. TMS offers an alternative modality to treat depression for patients who are partially responsive to drug treatment, can’t take depression medications, or are not eligible to receive ECT or had significant side effects from ECT in the past.
“When you’re talking about depression in the mild-to-moderate range, that’s something where TMS for a lot of people could be a reasonable treatment option,” said Dr. Wu. “We don’t want people to think of TMS as a ‘treatment of last resort’.”
Dr. Wu and his team at Northwest D.C. have completed treatment of one patient earlier this fall and started the rTMS therapy on a second patient a few weeks ago. MAPMG’s first rTMS patient reported a significant improvement in alleviating a depressive episode, reducing a pre-treatment PHQ-9 score from 15 to 3 over the course of the treatment.
The treatment occurs over a four to six week period each weekday, lasting approximately 40 minutes for each treatment (one hour total clinic time). There are basic treatment parameters, but an ongoing study is looking a further refinement.
If a patient meets the criteria of a major depressive episode, a behavioral health nurse will refer the patient to a psychiatrist, who will perform an evaluation and can make a referral to Dr. Wu for rTMS treatment. Treating psychiatrists need to complete a TMS referral smart phrase referral in KP HealthConnect, and can schedule the appointment in eConsult.




